Doctors Expect to Use Telehealth More Extensively Post COVID-19
AUTHORS
Chris Jaeger, MD, MBA
Former Vice President, Care Redesign & Chief Clinical Innovation Officer
Former Vice President, Care Redesign & Chief Clinical Innovation Officer

Physicians Embracing Telehealth During Pandemic
Telehealth is quickly emerging as an important clinical tool for physicians scrambling to adapt to the COVID-19 pandemic. Both patients and physicians report being happy with treatment delivered via telehealth, but doctors say barriers to adoption still exist.
Two April surveys conducted by the Pacific Business Group on Health’s California Quality Collaborative, during a webinar with independent physician associations (IPAs), community health clinics and managed services organizations, found that more than 80% of polled physician practices in California are presently using telehealth to deliver care.
Most practices report having launched telehealth services in earnest only in the three-to-four weeks after the pandemic’s shelter-in-place orders rolled out. Providers are using a combination of both telephone and video technologies not only for COVID-19 patient screening, but also urgent care, wellness visits and other clinical services.
Nearly three-quarters of poll respondents said clinicians were satisfied or very satisfied with providing care via telehealth.
Nonetheless, uncertainties remain about payment, policy and patient uptake of this technology. About one-third of respondents said policies on payment for telehealth were confusing or very confusing, and 64% said they need more guidance from health plans on billing.
Notably, about 40% of IPA representatives said they were extremely or very worried about their organizations’ financial health, while another 47% said they were somewhat worried.
During CQC’s webinars, IPAs and small physician practices identified a range of additional barriers to launching or expanding telehealth, including:
- Helping patients adopt telehealth, notably older patients without smartphones or with low digital literacy
- Reaching hard-to-find patients, like homeless patients without phones
- Improving patient acceptance and technical training (providers did note that when patients tried telehealth, they generally liked it)
- Providing staff training
- Documenting and coding for telehealth visits
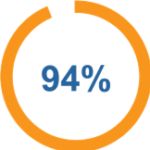
Despite the challenges, there’s broad agreement that the COVID-19 epidemic has helped to push past resistance to the more widespread use of telehealth; 94% of IPA respondents tell PBGH that they expect to use telehealth differently or more extensively once the pandemic begins to abate.



